By Tami S. Scott
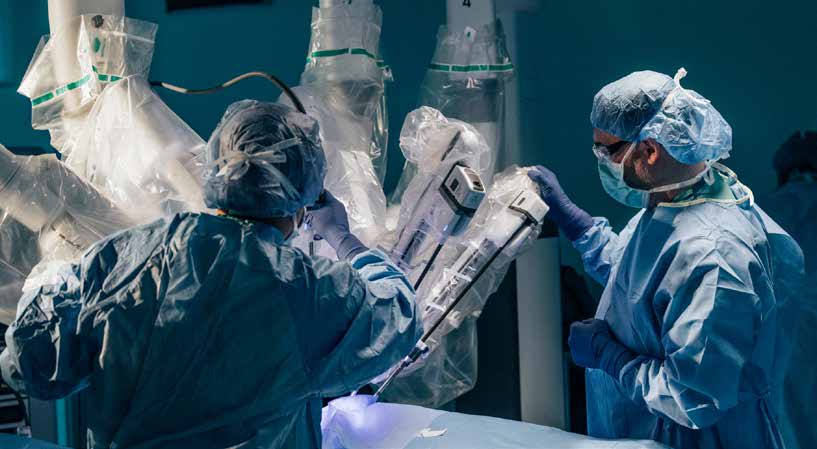
For Dr. Lin Wang, who practices general, laparoscopic, and robotic surgery, having a da Vinci® computer-enhanced surgical system at her disposal was critical in her decision-making to join the team at St. Peters Health Partners in Albany.
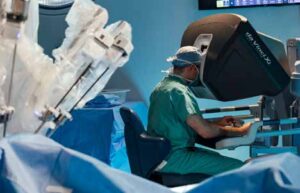
 “If I could, I would spend most of my time in the operating room on the da Vinci,” said Wang, who is with St. Peter’s Hepatobiliary, Pancreatic, and General Surgery, a practice of St. Peter’s Health Partners Medical Associates. “I would not work at a place that did not have a robot.”
“If I could, I would spend most of my time in the operating room on the da Vinci,” said Wang, who is with St. Peter’s Hepatobiliary, Pancreatic, and General Surgery, a practice of St. Peter’s Health Partners Medical Associates. “I would not work at a place that did not have a robot.”
Those sentiments reflect the position of many surgeons who are now completing their residency programs fully trained in performing minimally invasive surgeries, including robotic procedures.
The benefits are vast for both doctors and patients – less complications, less scarring, and quicker recoveries.
 The Capital Region is fortunate to be the home of two hospitals within St. Peter’s Health Partners to have secured five da Vinci surgical systems: four located at St. Peter’s Hospital in Albany and one at Samaritan Hospital in Troy.
The Capital Region is fortunate to be the home of two hospitals within St. Peter’s Health Partners to have secured five da Vinci surgical systems: four located at St. Peter’s Hospital in Albany and one at Samaritan Hospital in Troy.
St. Peter’s Hospital has been in the forefront of robotic surgery, being the first hospital in the Capital Region to acquire the technology in 2004.
Since then, St. Peter’s and Samaritan hospitals combined have performed the greatest number of robotic procedures in the Capital Region with more than 22,000 to date. Pioneers in this latest and most advanced type of minimally invasive surgery, they are also national leaders: St. Peter’s Hospital ranks in the top 1% of total robotic surgery volume across more than 2,400 hospitals in the United States.
So, what exactly is robotic surgery and how does it relate and differ from other minimally invasive surgeries such as laparoscopy and advanced endoscopy? First, minimally invasive surgeries are performed by making small incisions and with surgeons using a camera with console and long instruments to do the actual surgery. They have become more and more routine over the last 20 years.
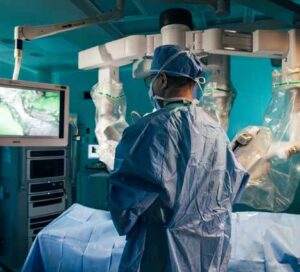
“Probably the first progression from open surgery to minimally invasive surgery would have been laparoscopy,” said Dr. Nicholas Montalto, chief medical officer for acute care, St. Peter’s Health Partners. “The da Vinci robot, the computer-assisted surgery, is a progression from laparoscopy.”
The surgical system integrates robotics and extremely sophisticated computer technology with the skills of the surgeon. It allows the surgeon to perform delicate operations with great precision and maneuverability but requiring only tiny surgical openings.
“Because the robot allows us better dexterity, the camera can potentially allow us better visualization compared to minimally invasive,” Dr. Wang said. “Instead of seeing in two-dimensional image [like with laparoscopy, for instance], we have binocular vision when we work through the robot.”
Also, straight instruments with basic capabilities are replaced with the robot’s “extra wrist” that can “turn in a way that we wouldn’t normally be able to do with laparoscopic instruments,” she added. “I think for a lot of surgeons, it helps us to do certain dissections in a much more ergonomic way.”
Worthy to note is that the term “robotic” often misleads people to believe that the robot is performing the surgery.
“The machine doesn’t do anything that the surgeon isn’t doing,” Dr. Montalto said. “It’s computer-assisted surgery. The visualization is superior, and the movement of the instruments is superior.”
Robotic procedures encompass several different surgical specialty areas, such as general surgery, colorectal, gynecological oncology, gynecology, hepatobiliary and pancreatic, urology, and thoracic.
“It’s a wonderful tool that has improved laparoscopy tenfold with wristed instruments, with visualization, with postoperative recovery – I think it’s a wonderful tool for all of our patients,” said Dr. Barbara Brazis, chief of robotic surgery at St. Peter’s Health Partners.
She hopes administration throughout the country will make it a priority to find ways to make these surgeries accessible to all.
“The length of [hospital] stay is far decreased after robotic than open surgery and sometimes even laparoscopic. There are some specialties where you can take the length of stay from 10 days down to two days – that’s a huge savings for the hospital. Right there the robot would pay for itself,” Dr. Brazis said.
When asked if insurance companies can be a barrier for robotic procedures, Dr. Montalto said not anymore.
“About 10 years ago, especially in the gynecology field, there were a couple of insurance companies that would not pay for the surgery to be done robotically versus laparoscopically or open, because the literature didn’t show a definite advantage in terms of mortality or serious complications by using the robot,” Montalto said. “They didn’t consider that there was any advantage – that’s not the case anymore. I haven’t encountered that in years as robotics has become so popular … There’s a tremendous number of advantages from robotics that I think the insurance companies weren’t necessarily appreciating.”
In the field of gynecological oncology, robotic surgery has had a wide impact.
“Robotic surgery has dramatically improved gynecologic oncology care,” said Dr. Joyce Barlin, a surgeon with Women’s Cancer Care Associates in Albany. “Robotic surgery offers superior visualization along with articulation of instruments to assist in the challenging dissection often required for oncologic surgery.”
In fact, more patients are becoming knowledgeable about robotic procedures and how it can help them in the recovery process.
“Patients are often aware of robotic surgery prior to their initial consultation and are grateful that robotic surgery is available through our Women’s Cancer Care Associates practice at St. Peter’s Hospital,” Barlin said. “Most of our patients undergoing major surgery using the robotic platform are able to safely go home on the same day of surgery.”
Is robotic surgery the future for all surgeries?
Dr. Rebecca Keim, a general surgeon with St. Peter’s Hepatobiliary, Pancreatic, and General Surgery, specializes in hepatobiliary and pancreatic cases. She was already in practice when she chose to train in robotic surgery and now performs about 100 surgeries per year with the da Vinci. This estimate is in addition to about 150 laparoscopic cases she performs per year.
“As we have more time for robotics, people are switching more and more from laparoscopic to robotic if there’s availability to do so,” she said.
However, Dr. Keim still performs traditional open techniques, which tend to be “large cancer cases that aren’t amenable to robotics or are just too complex.” She explained the dual efforts of docking and undocking the robot when necessity calls. For example, if Dr. Keim is working with the da Vinci on a cancer case for hours due to a tumor factor and the surgical team is not progressing, they can simply undock the robot, she scrubs in, and they do the case bedside.
“There’s times, too, when you go back and forth,” Keim added. “There’s times when we come bedside, we take out a specimen like a tumor, and then we redock the robot again and finish the operation.”
“I don’t think that minimally invasive or robotic surgery could ever replace everything that we do open,” Dr. Wang said. “There’s always a role for open surgery. Again, depending on the situation, it tends to be for more emergent type situations, where there’s not time to dock a robot or get those instruments in. Open surgery will always be there as an option.”
Dr. Brazis also agreed that open surgery will always have a place in the operating room.
“First of all, there are some people who aren’t trained in robotics and some surgeries are deemed to require open surgery in some specialties … so open surgeries are still done very often,” she said.
Again, St. Peter’s and Samaritan hospitals have five da Vinci surgical robotic systems to date. Donors have helped play a crucial role in the program by providing philanthropic support for the purchase and use of the surgical systems at St. Peter’s Health Partners.
“More and more surgeons coming out of residency programs and fellowship programs are trained on the da Vinci robot versus 10 years ago when they weren’t,” Montalto said.
And if they’re not skilled in it but would like to be, there is a comprehensive training pathway that includes several components, including system orientation with Intuitive, the company that makes the da Vinci robot, as well as hands-on training, and a proctoring program.
Dr. Keim said she believes the future of surgery will involve training people who can perform open, laparoscopic, and robotic surgery, which will in turn extend the training periods.
“It’s a big paradigm shift and you really have to be facile at all techniques when taking care of patients,” Keim said.
She said she thinks hospital leaders understand the need to support surgeons who want to use robotics. Though there’s a significant expense, they will find a way financially that makes sense.
“I think in 10 years, the costs are going to drop because [robotics] is going to become so common. I think other companies are going to get in the mix and allow it to become more affordable, she said.
A drop in cost aligns more with Dr. Montalto’s way of thinking, which is that robotics is the future of all surgery.
“There are programs that have only robotic surgery – every single case is done robotically, and they run the robot 24 hours a day, seven days a week, 365 days a year,” he said. “A goal for our program will be to do that also because one of the limitations of robotics is only being able to do it during business hours.” Staff on evenings and weekends may not be as proficient with robotics, so training all staff is vital for treating patients with the same opportunities for care.
 “I think it doesn’t give the patient the optimal care if you can’t offer robotic surgery around the clock,” Dr. Montalto said. “The time of day shouldn’t matter.”
“I think it doesn’t give the patient the optimal care if you can’t offer robotic surgery around the clock,” Dr. Montalto said. “The time of day shouldn’t matter.”


 Definition: “Community paramedicine is a relatively new and evolving healthcare model. It allows paramedics and emergency medical technicians (EMTs) to operate in expanded roles by assisting with public health and primary healthcare and preventive services to underserved populations in the community.” Rural Health Information Hub
Definition: “Community paramedicine is a relatively new and evolving healthcare model. It allows paramedics and emergency medical technicians (EMTs) to operate in expanded roles by assisting with public health and primary healthcare and preventive services to underserved populations in the community.” Rural Health Information Hub Like most other organizations, healthcare facilities have moved toward total digitization. The major benefit of this change is that it has provided an efficient way of sharing patient records among healthcare professionals. Compared to paper-based records, electronic health records require less workforce, time, and physical storage.
Like most other organizations, healthcare facilities have moved toward total digitization. The major benefit of this change is that it has provided an efficient way of sharing patient records among healthcare professionals. Compared to paper-based records, electronic health records require less workforce, time, and physical storage. Peace of mind is paramount for healthcare providers. However, some physicians hesitate to report potential medical malpractice claims to their insurance carriers for fear of jeopardizing their coverage. This article aims to clarify the importance of timely reporting and dispel common misconceptions.
Peace of mind is paramount for healthcare providers. However, some physicians hesitate to report potential medical malpractice claims to their insurance carriers for fear of jeopardizing their coverage. This article aims to clarify the importance of timely reporting and dispel common misconceptions.



 I have worked my entire career in government or nonprofits. It has led me to see the value of models that protect access to care for those who are underserved. The non profit model uses profits to re-invest in the provision of care in the community. Income is derived from profitable areas of care . Where the cost of care is not covered by insurance or there is no insurance, donors, grants and government subsidies often fill the gap.
I have worked my entire career in government or nonprofits. It has led me to see the value of models that protect access to care for those who are underserved. The non profit model uses profits to re-invest in the provision of care in the community. Income is derived from profitable areas of care . Where the cost of care is not covered by insurance or there is no insurance, donors, grants and government subsidies often fill the gap.
 Round two of the Grieving Families Act has slight changes but is substantially the same one vetoed by Gov. Kathy Hochul earlier this year, citing the need to evaluate the “impact of these massive changes to the economy, small businesses, individuals, the state’s complex healthcare system.”
Round two of the Grieving Families Act has slight changes but is substantially the same one vetoed by Gov. Kathy Hochul earlier this year, citing the need to evaluate the “impact of these massive changes to the economy, small businesses, individuals, the state’s complex healthcare system.”