
Open since May 2025, the practice takes an integrated approach to ensure patients and providers have streamlined access to medical records. This connectivity through the St. Peter’s Health Partners EMR makes care more seamless and communication easier.
 “Our goal is simple: to give patients access to the latest orthopedic innovations as we provide quality and efficient care centered around each patient’s needs,” said Imran Akhtar, DO, who founded the practice with Hamza Murtaza, MD.
“Our goal is simple: to give patients access to the latest orthopedic innovations as we provide quality and efficient care centered around each patient’s needs,” said Imran Akhtar, DO, who founded the practice with Hamza Murtaza, MD.
Accessibility
St. Peter’s Orthopedics in Latham has expanded from its two founders to a staff of six physicians and two advanced practice providers. Each doctor brings his own sub-specialty to the practice.
“That expansion is due to demand, but we also wanted to make sure we offer every sub specialty,” said Dr. Akhtar, DO. “Now we can provide comprehensive musculoskeletal care from the spine, shoulders, and hands, to hips, knees, foot and ankles.”
The orthopedic practice is a part of St. Peter’s Health Partners Medical Associates, which is a division of St. Peter’s Health Partners. The medical group includes more than 1,100 physicians and advanced practitioners in more than 130 locations around the Capital Region.
St. Peter’s Health Partners is the region’s largest and most comprehensive, notfor- profit network of high-quality, advanced medical care, primary care, rehabilitation, and senior services. It is a member of Trinity Health, one of the nation’s largest Catholic health systems, operating 92 hospitals in 25 states.

 Making It Easy for Patients
Making It Easy for Patients
Additionally, St. Peter’s Orthopedics offers an orthopedic walk-in clinic Mondays through Fridays from 8 a.m. to 4 p.m. at the Latham location.
“The clinic has been a huge draw where patients don’t have to schedule a visit or wait too long to see an orthopedic surgeon,” said Dr. Akhtar. “They can walk in, and we will see them.”
From the opening of the practice, it was important to build the services around the needs of the patients.
“From the beginning, we wanted to do things differently,” added Dr. Akhtar.
“We wanted to make sure patients never feel rushed.”
It was also important to offer a wide scope of services.
“We offer a one-stop shop where services are as accessible and convenient for people in their busy lives as we can make it,” added Kyle Angelicola Richardson, MD, whose orthopedic specialty is the upper extremity and wrist.
Team of Experts
The orthopedic team brings together exceptional expertise and experience to deliver the best possible outcomes. All surgeons are fellowship trained, bringing cutting-edge orthopedics to the practice’s patient-centered model. The specialists cover a wide range of care – from roboticassisted surgery to personalized ankle and foot care.
 Dr. Akhtar, who is board certified, specializes in joint replacement and reconstruction. He completed his residency in orthopedic surgery at the Oklahoma State University – Center for Health Sciences in Tulsa. After finishing his residency, he spent an additional year completing an American Association of Hip and Knee Surgeons Fellowship in Hip and Knee replacement at Desert Orthopedic Center in Las Vegas, Nevada. Dr. Akhtar specializes in minimally invasive hip replacement, which reduces the size of surgical scars and expedites postoperative recovery. He performs direct anterior hip replacements and has an interest in partial knee arthroplasty and robotic assisted knee replacement. “My approach to medicine is rooted in empathy and respect. I treat every patient as I would want my own family to be treated. Listening is at the heart of my practice,” Dr. Akhtar said. “By truly hearing my patients’ concerns, we can build a personalized and effective care plan that supports their recovery and long-term well-being.”
Dr. Akhtar, who is board certified, specializes in joint replacement and reconstruction. He completed his residency in orthopedic surgery at the Oklahoma State University – Center for Health Sciences in Tulsa. After finishing his residency, he spent an additional year completing an American Association of Hip and Knee Surgeons Fellowship in Hip and Knee replacement at Desert Orthopedic Center in Las Vegas, Nevada. Dr. Akhtar specializes in minimally invasive hip replacement, which reduces the size of surgical scars and expedites postoperative recovery. He performs direct anterior hip replacements and has an interest in partial knee arthroplasty and robotic assisted knee replacement. “My approach to medicine is rooted in empathy and respect. I treat every patient as I would want my own family to be treated. Listening is at the heart of my practice,” Dr. Akhtar said. “By truly hearing my patients’ concerns, we can build a personalized and effective care plan that supports their recovery and long-term well-being.”

 Dr. Murtaza brings his expertise in hip and knee surgery to the orthopedic team. He received his medical degree from SUNY Upstate Medical University in Syracuse. He completed a residency in orthopedics at Albany Medical Center, followed by a fellowship in adult reconstruction at NYU Langone Hospital in New York City.
Dr. Murtaza brings his expertise in hip and knee surgery to the orthopedic team. He received his medical degree from SUNY Upstate Medical University in Syracuse. He completed a residency in orthopedics at Albany Medical Center, followed by a fellowship in adult reconstruction at NYU Langone Hospital in New York City.
He specializes in both primary and complex hip and knee replacements, and is adept at hip surgery, especially the direct anterior approach to optimize patient recovery. He also specializes in total and partial knee replacement, revision hip and knee surgeries, and general trauma injuries.
“There is no greater feeling than to see a patient come in, and over time, make the transition from a wheelchair to a walker to a cane, and then walking independently,” said Dr. Murtaza. “It has to be one of the more gratifying things to experience in all honesty. That’s the foundation of patient care.”
Dr. Angelicola-Richardson, who is boardcertified, focuses on issues of the upper extremity and wrist. He is a graduate of SUNY Upstate Medical University in Syracuse. He completed his orthopedic surgery residency at Albany Medical Center, where he gained extensive experience in trauma and reconstructive procedures. He further honed his skills through a prestigious fellowship in hand and upper extremity surgery at New York-Presbyterian/Columbia University Irving Medical Center in New York City, one of the nation’s leading programs in this specialty. He spent time at St. Peter’s during his residency, so he knew of the highquality, compassionate care offered by the clinicians at St. Peter’s.
 “It is an outstanding organization,” Dr. Angelicola Richardson said, “but, most importantly, the quality of care and the commitment to the community align with my responsibilities to my patients.” Before joining St. Peter’s Orthopedics, Dr. Angelicola-Richardson served patients at Rome Health in Rome, New York, where he was known for his compassionate care and meticulous surgical outcomes.
“It is an outstanding organization,” Dr. Angelicola Richardson said, “but, most importantly, the quality of care and the commitment to the community align with my responsibilities to my patients.” Before joining St. Peter’s Orthopedics, Dr. Angelicola-Richardson served patients at Rome Health in Rome, New York, where he was known for his compassionate care and meticulous surgical outcomes.
Kevin McCracken, MD, who is boardcertified, leads the spine care team. He has worked two decades as a spine surgeon, first at his own practice in New Jersey and then in Florida.
“St. Peter’s has everything I was looking for: the mission statement of providing for the community, plus working with a group of people covering every specialty,” he said. “We can treat the whole gamut; every aspect of care.”
In addition to his extensive surgical and academic training, McCracken has broad experience in the treatment of
adult and adolescent patients with spine disorders. McCracken firmly believes in his mission to care for each individual patient and their total well-being, taking pride in providing compassionate, understanding, and supportive care.
Over the past 25 years, he has completed more than 10,000 spine procedures ranging from minimally invasive procedures to complex reconstructive surgery for scoliosis and spinal deformity. He also has served as a spine trauma surgeon at a Level 1 Trauma Center for over 10 years.
Adel Mahjoub, MD, manages the foot and ankle care team. He earned his medical degree from the University of Pittsburgh School of Medicine in 2019. He went on to complete a five-year orthopedic surgery residency at Cooper University Hospital in Camden, New Jersey, where he developed a strong interest in foot and ankle pathology. He then pursued advanced fellowship training in foot and ankle surgery at Harvard Massachusetts General Hospital in Boston, Massachusetts, completing his fellowship in 2024.
 Dr. Mahjoub’s clinical expertise spans the full spectrum of foot and ankle care. He has specialized training in minimally invasive techniques, ankle arthroscopy, ankle fusion, total ankle replacement, flatfoot reconstruction, and bunion correction. He also treats a wide range of tendon and soft tissue conditions, including disorders of the Achilles and peroneal tendons.
Dr. Mahjoub’s clinical expertise spans the full spectrum of foot and ankle care. He has specialized training in minimally invasive techniques, ankle arthroscopy, ankle fusion, total ankle replacement, flatfoot reconstruction, and bunion correction. He also treats a wide range of tendon and soft tissue conditions, including disorders of the Achilles and peroneal tendons.
“I focus on the care of sports injuries and arthritis, with an emphasis on minimally invasive techniques,” Dr. Mahjoub said. “It is deeply rewarding to apply my hands on skills to restore function, relieve pain, and support patients as they return to their daily lives.”
Board-certified Peter Shaughnessy, MD, leads the hand and wrist specialty program. He graduated valedictorian from the University at Buffalo School of Medicine and Biomedical Sciences and went on to complete his residency in orthopedic surgery at Dartmouth- Hitchcock Medical Center in New Hampshire. Dr. Shaughnessy then completed a fellowship in Hand and Upper Extremity Surgery at NYU Langone Health in New York City which included microvascular training.
Dr. Shaughnessy’s professional interests include complex upper extremity trauma, arthritic conditions of the hand and wrist, peripheral nerve surgery, and arthroscopy. He is board-certified and has more than 10 years of experience. “I wanted to join an employee owned orthopedic group,” Dr. Shaughnessy said, “and St. Peter’s is solidly behind us. The surgeons here can treat every orthopedic need. Our goal is to be a onestop shop for our patients. We’re excited for the future of orthopedics here and want everyone to know about it.”
Seamless Care
A huge component of delivering seamless patient care is communication, both verbally and electronically. The EMR at St. Peter’s Health Partners Medical Associates facilitates the in-house sharing of information.
The orthopedic team works closely with primary care providers and hospitals throughout the Capital Region to coordinate patient care.
“We use the same network the hospital uses, the same system the primary care network uses -so we have seamless communication,” Dr. Murtaza said. “If the primary care doctor has questions, they can text me or send me a message on the same EMR. That goes a long way toward coordinating care. It avoids unnecessary tests and delays in patient care.”
Additionally, patients can access their medical records through Trinity Health’s MyChart application which is part of the EMR. This allows patients to make appointments, get test results, and communicate with their provider. The app can be accessed via the St. Peter’s website www.sphp.com/mychart.
Surgery and Rehabilitation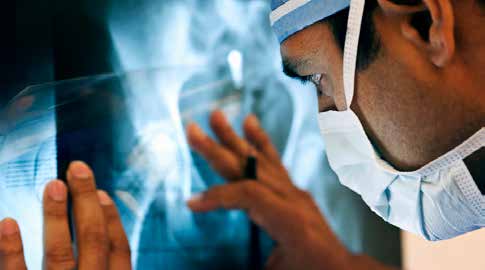 The surgical team uses the latest technologies and techniques to treat patients effectively. That means robotic assisted techniques for joint replacements, minimally invasive procedures, and advanced diagnostics.
The surgical team uses the latest technologies and techniques to treat patients effectively. That means robotic assisted techniques for joint replacements, minimally invasive procedures, and advanced diagnostics.
Not every orthopedic condition requires surgery. St. Peter’s Orthopedics follows a specific protocol for every patient: evaluation, therapy first, surgery when needed, and recovery and support. Non surgical options include joint disease treatment, physical therapy and rehabilitation, interventional pain management, bone health, platelet-rich plasma, shockwave, and electromyography.
 St. Peter’s Orthopedics works with Sunnyview Rehabilitation, which has 12 outpatient clinics throughout Albany, Saratoga, Schenectady, and Renssalaer counties, and is a member of St. Peter’s Health Partners.
St. Peter’s Orthopedics works with Sunnyview Rehabilitation, which has 12 outpatient clinics throughout Albany, Saratoga, Schenectady, and Renssalaer counties, and is a member of St. Peter’s Health Partners.
Care at Sunnyview differs from most other physical therapy offices in at least two ways – a therapist will work with a patient one-on-one and, if needed, will treat a patient in their home.
“Every area of orthopedics relies on physical therapy. They truly work hand in hand. I tell my patients that therapy is often underutilized,” Dr. Murtaza said. “With consistency, physical therapy can ease many problems and help people improve without medication or surgery.” When surgery is the only remaining option, the surgeons at St. Peter’s Orthopedics are eager to help patients recover and get back to living their lives. “I love a practice where you are able to deliver care and see results pretty much right away,” said Dr. Akhtar. “After a fracture, you can set their broken bone and help them get moving again. You feel a little sense of accomplishment that you contributed to that healing.”
The physicians at St. Peter’s Orthopedics also meet regularly, to collaborate and share their expertise to maximize patient experience and outcomes.
“For those patients who have complicated and multiple issues, it’s very important that we communicate between staff and physicians,” said Dr. Angelicola-Richardson. “We maintain an open line of communication and that helps patients feel welcome and heard.”
St. Peter’s Orthopedics is located at 1182 Troy Schenectady Road, Suite 100, Latham. You may reach them at (518) 269-4690. Regular office hours are Monday through Friday, 8 a.m. to 4:30 p.m., and walk-in clinic hours are Monday through Friday, 8 a.m. to 4 p.m.


 I will not debate the politics behind the recent health care cuts, but I will share my concerns about their impacts.
I will not debate the politics behind the recent health care cuts, but I will share my concerns about their impacts.

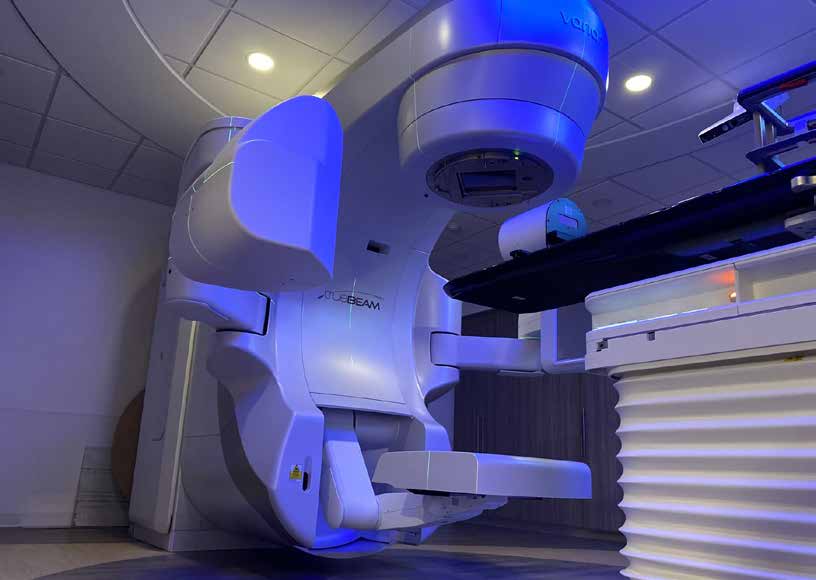
 Dr. Korytko said that in the last five years, the radiation oncology field has seen a big increase in the types of radiopharmaceutical drugs available for cancer treatment. He highlighted two drugs specifically that are available at Bassett: Lutathera, a special treatment for neuroendocrine cancer, and Pluvicto, a radioactive IV treatment used for prostate cancer. Dr. Korytko shared that patients come to Bassett for these kinds of treatment options, and he said the rural setting helps the team provide the best care for patients.
Dr. Korytko said that in the last five years, the radiation oncology field has seen a big increase in the types of radiopharmaceutical drugs available for cancer treatment. He highlighted two drugs specifically that are available at Bassett: Lutathera, a special treatment for neuroendocrine cancer, and Pluvicto, a radioactive IV treatment used for prostate cancer. Dr. Korytko shared that patients come to Bassett for these kinds of treatment options, and he said the rural setting helps the team provide the best care for patients. “We’re giving novel therapies, which sets us apart from just being a rural hospital that provides the basics. We were one of the earliest sites giving Lutathera and Pluvicto. We have a team that’s very committed to bringing the best care we can to our patients. And we treat them in a place that’s a comfortable, community based treatment location. You could go to a larger, metropolitan center and get lost in the traffic and crowds, or you can come here and get treated a little bit more like family. To be able to offer this type of care here is really a testament to our investment in doing the right thing,” said Dr. Korytko.
“We’re giving novel therapies, which sets us apart from just being a rural hospital that provides the basics. We were one of the earliest sites giving Lutathera and Pluvicto. We have a team that’s very committed to bringing the best care we can to our patients. And we treat them in a place that’s a comfortable, community based treatment location. You could go to a larger, metropolitan center and get lost in the traffic and crowds, or you can come here and get treated a little bit more like family. To be able to offer this type of care here is really a testament to our investment in doing the right thing,” said Dr. Korytko. “We’re involved in radiation clinical trials using an investigational radiation implant to treat skin cancer,” Dr. Korytko stated. “We’ve been enrolling patients in a study for recurrent skin cancer who have limited treatment options. We’re one of the first sites in the country to be involved in this clinical trial and are the first in the U.S. to open a clinical trial investigating this device in treating pancreatic cancer.”
“We’re involved in radiation clinical trials using an investigational radiation implant to treat skin cancer,” Dr. Korytko stated. “We’ve been enrolling patients in a study for recurrent skin cancer who have limited treatment options. We’re one of the first sites in the country to be involved in this clinical trial and are the first in the U.S. to open a clinical trial investigating this device in treating pancreatic cancer.” The team of over 100 diverse staff members at Bassett Cancer Institute is comprised of nurses (including clinic nurses, infusion nurses, and nurse navigators), support staff (including social workers, financial counselors, nutritionists, and administrative staff) and radiation therapists. Anush Patel, MD, Chief of Medical Oncology and Hematology, shared how patients recognize the high-quality care offered by this multidisciplinary team.
The team of over 100 diverse staff members at Bassett Cancer Institute is comprised of nurses (including clinic nurses, infusion nurses, and nurse navigators), support staff (including social workers, financial counselors, nutritionists, and administrative staff) and radiation therapists. Anush Patel, MD, Chief of Medical Oncology and Hematology, shared how patients recognize the high-quality care offered by this multidisciplinary team. makes us stand out in the area, and even at the national level, that we are providing fantastic care in a rural setting,” said Dr. Patel, who also highlighted the unique transportation support system offered at Bassett, which helps ensure patients who face transportation challenges across the health system’s rural communities can come from their homes to the cancer center for appointments and treatments.
makes us stand out in the area, and even at the national level, that we are providing fantastic care in a rural setting,” said Dr. Patel, who also highlighted the unique transportation support system offered at Bassett, which helps ensure patients who face transportation challenges across the health system’s rural communities can come from their homes to the cancer center for appointments and treatments. “We are trained especially in noncancerous blood disorders, along with malignant hematology, which is leukemia and lymphoma, as well as medical oncology, which involves solid tumors. It’s quite seamless because someone who gets chemotherapy might have a complication of low blood count, so we need to be quite well trained and comfortable with dealing with the anticipated complications,” explained Dr. Patel.
“We are trained especially in noncancerous blood disorders, along with malignant hematology, which is leukemia and lymphoma, as well as medical oncology, which involves solid tumors. It’s quite seamless because someone who gets chemotherapy might have a complication of low blood count, so we need to be quite well trained and comfortable with dealing with the anticipated complications,” explained Dr. Patel.  “Gynecologic oncology is a very specialized surgical subspecialty, so patients in rural areas can be very underserved and must travel very far for care. It’s rare to have a local, full-service, specially trained gynecologic oncologist practice here in Cooperstown and in the surrounding communities. With all the therapies we provide, between surgery visits, chemotherapy, radiation and more, our relationship with patients isn’t a one-time point of care. That’s a big reason why it’s such a benefit to have localized care in a smaller center with more focus on patients and their needs,” said Dr. Pelkofski.
“Gynecologic oncology is a very specialized surgical subspecialty, so patients in rural areas can be very underserved and must travel very far for care. It’s rare to have a local, full-service, specially trained gynecologic oncologist practice here in Cooperstown and in the surrounding communities. With all the therapies we provide, between surgery visits, chemotherapy, radiation and more, our relationship with patients isn’t a one-time point of care. That’s a big reason why it’s such a benefit to have localized care in a smaller center with more focus on patients and their needs,” said Dr. Pelkofski.
 “We’re kind of outgrowing our space, so we’re investing in a new cancer center by building out and expanding the oncology unit inside FoxCare Center,” stated Dr. Tinger. “The plan is to expand the space, so we’ll have more room for offices and exam rooms, including private rooms for infusions. We have pending plans for expansion in our other offices, as well.”
“We’re kind of outgrowing our space, so we’re investing in a new cancer center by building out and expanding the oncology unit inside FoxCare Center,” stated Dr. Tinger. “The plan is to expand the space, so we’ll have more room for offices and exam rooms, including private rooms for infusions. We have pending plans for expansion in our other offices, as well.” As the teams and the locations grow, however, the mission of Bassett Cancer Institute, as described by Dr. Tinger, will remain the same: “Our mission is to take great care of patients with cancer. Hearing you have a cancer diagnosis puts someone in a very vulnerable position. We exist to remove the vulnerabilities and give people hope.”
As the teams and the locations grow, however, the mission of Bassett Cancer Institute, as described by Dr. Tinger, will remain the same: “Our mission is to take great care of patients with cancer. Hearing you have a cancer diagnosis puts someone in a very vulnerable position. We exist to remove the vulnerabilities and give people hope.”  Soon J. Park, MD, renowned both locally and internationally for his expertise and scientific contributions to cardiothoracic surgery, has joined the Albany Med Health System. He will serve as surgical director of cardiovascular services at Albany Medical Center, and he will collaborate with colleagues across the System to elevate a coordinated, regional approach to cardiovascular care.
Soon J. Park, MD, renowned both locally and internationally for his expertise and scientific contributions to cardiothoracic surgery, has joined the Albany Med Health System. He will serve as surgical director of cardiovascular services at Albany Medical Center, and he will collaborate with colleagues across the System to elevate a coordinated, regional approach to cardiovascular care. Obesity is a major chronic disease affecting many adults in the United States. At St. Peter’s Health Partners, the St. Peter’s Bariatric and Metabolic Care team treat obese and overweight patients in the greater Albany area, from Saratoga County, to Vermont, Western Massachusetts and even as far South as Poughkeepsie. Working out of both Samaritan Hospital and St. Peter’s Hospital, the multidisciplinary team includes providers specializing in bariatric surgery, internal and bariatric medicine, nutrition, and behavioral health to support a full range of individualized care for bariatric patients.
Obesity is a major chronic disease affecting many adults in the United States. At St. Peter’s Health Partners, the St. Peter’s Bariatric and Metabolic Care team treat obese and overweight patients in the greater Albany area, from Saratoga County, to Vermont, Western Massachusetts and even as far South as Poughkeepsie. Working out of both Samaritan Hospital and St. Peter’s Hospital, the multidisciplinary team includes providers specializing in bariatric surgery, internal and bariatric medicine, nutrition, and behavioral health to support a full range of individualized care for bariatric patients. For many patients experiencing obesity, bariatric surgery is selected as the best strategy to help them reach their targeted weight loss. At St. Peter’s Bariatric and Metabolic Care, patients are required to receive several clearances to qualify for surgery, which helps to ensure patients are ready and can be as successful as possible. Prior to receiving a date for surgery, patients must achieve 5% weight loss, receive clearances from nutrition, behavioral health, and cardiology, have an endoscopy and possibly also a sleep study. To be considered for surgery, patients need to have a BMI (body mass index) of 35-40 or higher and may need to have at least one of the comorbidities associated with obesity, including diabetes, high blood pressure, sleep apnea and high cholesterol.
For many patients experiencing obesity, bariatric surgery is selected as the best strategy to help them reach their targeted weight loss. At St. Peter’s Bariatric and Metabolic Care, patients are required to receive several clearances to qualify for surgery, which helps to ensure patients are ready and can be as successful as possible. Prior to receiving a date for surgery, patients must achieve 5% weight loss, receive clearances from nutrition, behavioral health, and cardiology, have an endoscopy and possibly also a sleep study. To be considered for surgery, patients need to have a BMI (body mass index) of 35-40 or higher and may need to have at least one of the comorbidities associated with obesity, including diabetes, high blood pressure, sleep apnea and high cholesterol. “About ten years ago, medical society made a shift toward minimally invasive surgery and shorter hospital stays which have dramatically improved patient outcomes,” said Dr. Hykin. “Right now, I complete a gastric sleeve surgery in three to five small incisions, and a gastric bypass is done in four to five small incisions. Patients can be in and out relatively quickly and get back to their everyday lives without much interruption.”
“About ten years ago, medical society made a shift toward minimally invasive surgery and shorter hospital stays which have dramatically improved patient outcomes,” said Dr. Hykin. “Right now, I complete a gastric sleeve surgery in three to five small incisions, and a gastric bypass is done in four to five small incisions. Patients can be in and out relatively quickly and get back to their everyday lives without much interruption.”
 “The process is about patient safety, protocolizing your approach, low complication rates, quality follow-up care – all of that combined. If you meet the bar, you’re granted Center of Excellence status, and you must recertify every three years. During those next three years you need to continue to meet the standards you were originally qualified by, and the ASMBS reviews
“The process is about patient safety, protocolizing your approach, low complication rates, quality follow-up care – all of that combined. If you meet the bar, you’re granted Center of Excellence status, and you must recertify every three years. During those next three years you need to continue to meet the standards you were originally qualified by, and the ASMBS reviews 

 meet patients wherever they’re ready to make changes. I’m all about sustainability and being realistic with where the patient currently is and what changes they want to make,” she said.
meet patients wherever they’re ready to make changes. I’m all about sustainability and being realistic with where the patient currently is and what changes they want to make,” she said. “Our office is truly based in a multidisciplinary approach,” Kontoh said. “We’re a very close office and we have very good communication with each other. We make sure we’re letting each of the other providers know if a patient may have a higher need for enhanced support as they work toward their goals. I also think the support groups we offer are a major highlight of our office – we cover topics ranging from binge eating to navigating change to the stress of the holiday season. The number of resources we offer is often surprising to patients.”
“Our office is truly based in a multidisciplinary approach,” Kontoh said. “We’re a very close office and we have very good communication with each other. We make sure we’re letting each of the other providers know if a patient may have a higher need for enhanced support as they work toward their goals. I also think the support groups we offer are a major highlight of our office – we cover topics ranging from binge eating to navigating change to the stress of the holiday season. The number of resources we offer is often surprising to patients.” Although each provider or team of specialists at St. Peter’s approaches bariatric medicine through a different lens, a common thread that connects them all is how rewarding they each find it when they can celebrate their patients’ successes alongside them. For each, overcoming obesity is less about the number on the scale and more about the unique and often seemingly simple achievements that affect each patient’s life in different ways.
Although each provider or team of specialists at St. Peter’s approaches bariatric medicine through a different lens, a common thread that connects them all is how rewarding they each find it when they can celebrate their patients’ successes alongside them. For each, overcoming obesity is less about the number on the scale and more about the unique and often seemingly simple achievements that affect each patient’s life in different ways.